Patient Safety
Patient safety is the foundation of high-quality healthcare. Large numbers of patients are harmed or die each year because of unsafe care, or get injured inadvertently when seeking healthcare. Many patients die annually because of diagnostic mistakes. The World Health Organization states:
“Unsafe medications practices and medication errors are a leading cause of patient safety incidents across the world. Patient safety is a serious global public health issue. Estimates show that in developed countries as many as one in 10 patients is harmed while receiving hospital care” [World Health Organization, September 14, 2016].
A great deal of the work identifying patient safety and practices that prevent harm have centered on adverse outcomes of care such as mortality and morbidity. Understanding the magnitude of the problem in hospitals and primary care facilities is the initial step on the way to improving patient safety.
What We’ve Done in Area of Patient Safety
Clinicians, hospitals, professional organizations, and scientists have made considerable advances during the last several years in improving patient safety. Improving healthcare outcomes is a top priority in clinical education and research studies. Prevention is the cornerstone of reducing medical errors and increasing patient well-being. Experts suggest that older methods to improving medical safety that was aimed at technical and structural improvements are important but do not explain all of the issues. Of course, technical and structural elements will remain necessary; however, the priority now is also on how individual healthcare providers execute their daily tasks, organizational procedures in the clinical setting, and communication across clinical healthcare teams are priorities among research studies.
What Are We Discovering About Patient Safety
Many patient safety practices, such as the use of simulators, bar coding, computerized physician order entry, and healthcare team resource management are considered key strategies to consider in order to avoid patient safety errors and improve healthcare processes. Research has explored these areas and further research is still needed. Additionally, an area of current investigation is how improvements using smart devices across the clinical setting affect how healthcare providers and administrators, operations, and procedures come together in the search for better patient outcomes.
Also, evidence-based principles of hospital design and style to increase safety and quality are also important. Specifically, how to prevent patient falls by supplying well-designed patient rooms and washrooms and creating decentralized nurses’ areas that permit quick access to patients. Other workplace design characteristics include reducing medication errors by supplying pharmacists with well-designed workspaces to allow them to complete prescriptions without distractions. These are just a few examples of emerging areas of study surrounding patient safety.
Handwashing Remains A Leading Intervention
Clean hands are the most effective protection from infection. Reducing infections through providing single bedrooms, improving air purification devices, and supplying numerous convenient places for hand washing are the mainstays of infection control. With a rise in drug-resistant microorganisms within all hospital settings, it is now significantly vital for healthcare employees to adhere to hand cleanliness guidelines. This may seem ‘old-school’; however, hand washing and the impact on reducing infections is still one of the single most effective strategies in patient safety.
Nurses are a Crucial to Patient Safety
Much of the patient safety research has focused on nurses. Importantly, nurses play an essential part in patient safety through their constant presence at the patient’s bedside. Nurses are essential to the surveillance and coordination that reduce adverse outcomes. However, staffing issues and suboptimal working conditions can impede nurses’ ability to detect and avoid negative events. Each added patient for every nurse, elevates the chances of nurses revealing poor or fair quality healthcare [Nurse Staffing, Education Affect Patient Mortality in Europe]. Similar outcomes such as high burnout, job dissatisfaction, and the work environment are all factors related to patient safety and must be addressed within each healthcare organization.
Other Healthcare Team Members
Sufficient and competent staffing are another area associated with quality care. Although clinicians’ intellectual biases play a part in many diagnostic mistakes, actual healthcare system issues also give rise to missed and delayed diagnoses, which is a large part of patient safety. Research has specifically suggested restricting shift length for medical residents as well as other hospital team members whenever possible. Research demonstrates severe and persistently fatigued medical residents are associated with are more errors. Suggested guidelines to reduce such errors include ensuring residents get sufficient sleep and comply with 80-hour workweek restrictions. Furthermore, residents, who perform 30-hour shifts must only take care of patients for approximately 16 hours and must have a 5-hour covered sleeping interval between 10 p.m. and 8 a.m. [Resident Duty Hours: Enhancing Sleep, Supervision, and Safety]
At-Risk Patient Safety Scenarios
Beyond the healthcare team, other elements are also key to improving patient safety. Being released from the hospital may be risky for patients. Almost 20% of patients experience an unfavorable event within the initial 21 days following discharge. These events include prescription medication problems, healthcare–associated microbe infections, and procedural difficulties. More often than not, fatalities following surgical procedures include the culmination of a stream of events. This begins with a primary complication that is accompanied by an increase and/or invasive type of patient care, which leads to further complications and treatment resulting in a patient’s death. As previously stated, prevention is key to improved patient safety and is possible through monitoring processes that include identifying patients who are at particular risk, quickly determining possible negative events, together with preventing and recovering from potential medical errors.
Patient Data and Communication
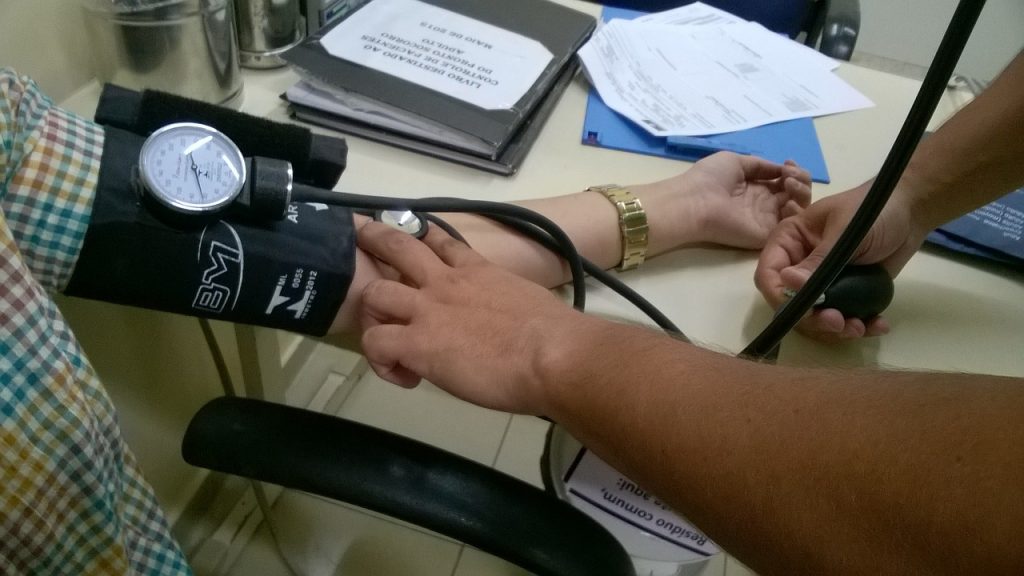
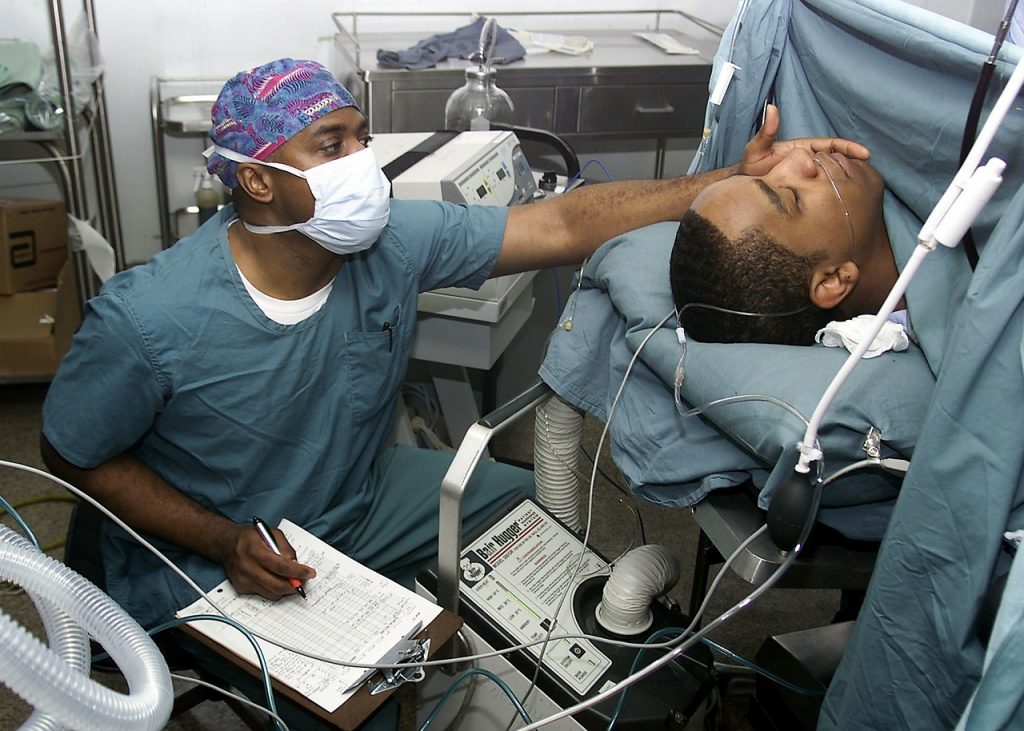
Pivotal to the overall impact of all elements regarding patient safety is patient data and information. The tracking procedures focus mainly on paying attention to, measuring, and documenting biological parameters including vital signs and laboratory values. On the other hand, surveillance information consists of not just physiological data but the integration of knowledge from members of the patient’s family, the clinical care team, medical databases, and healthcare support systems.
An individual on the healthcare team collects and records the relevant patient data, which is then used by all members of the team to look at the overall context of the patient and plan of care. Importantly, the information must be shared and reviewed across the team. These structures and procedures incorporate monitoring checklists, clinical information systems, and medical decision-support methods. Information is key and effective communication essential to reducing medical errors thus, improving patient safety. Educating clinicians and healthcare staff to communicate effectively as a team is a top priority to improve patient safety.
Conclusion
Recommendations for continued and future research dedicated to improving healthcare and patient safety requires a greater focus on how people, process, and practice combine inpatient care, as opposed to just on technical or structural enhancements. Patient safety is an evolving process. The creation and implementation of patient safety policies and procedures will continue. Patient safety requires resources and the support of the organization. A good patient safety officer knows when and how to select the approach to problem solving and change that can best impact a given situation positively and improve outcomes for patients. The Handbook of Patient Safety Compliance: A Practical Guide for Health Care Organizations is an excellent resource.